
Final ID: Poster #: SCI-057
Proximal Humerus Fractures in Children: Distribution and Predictors of Surgery
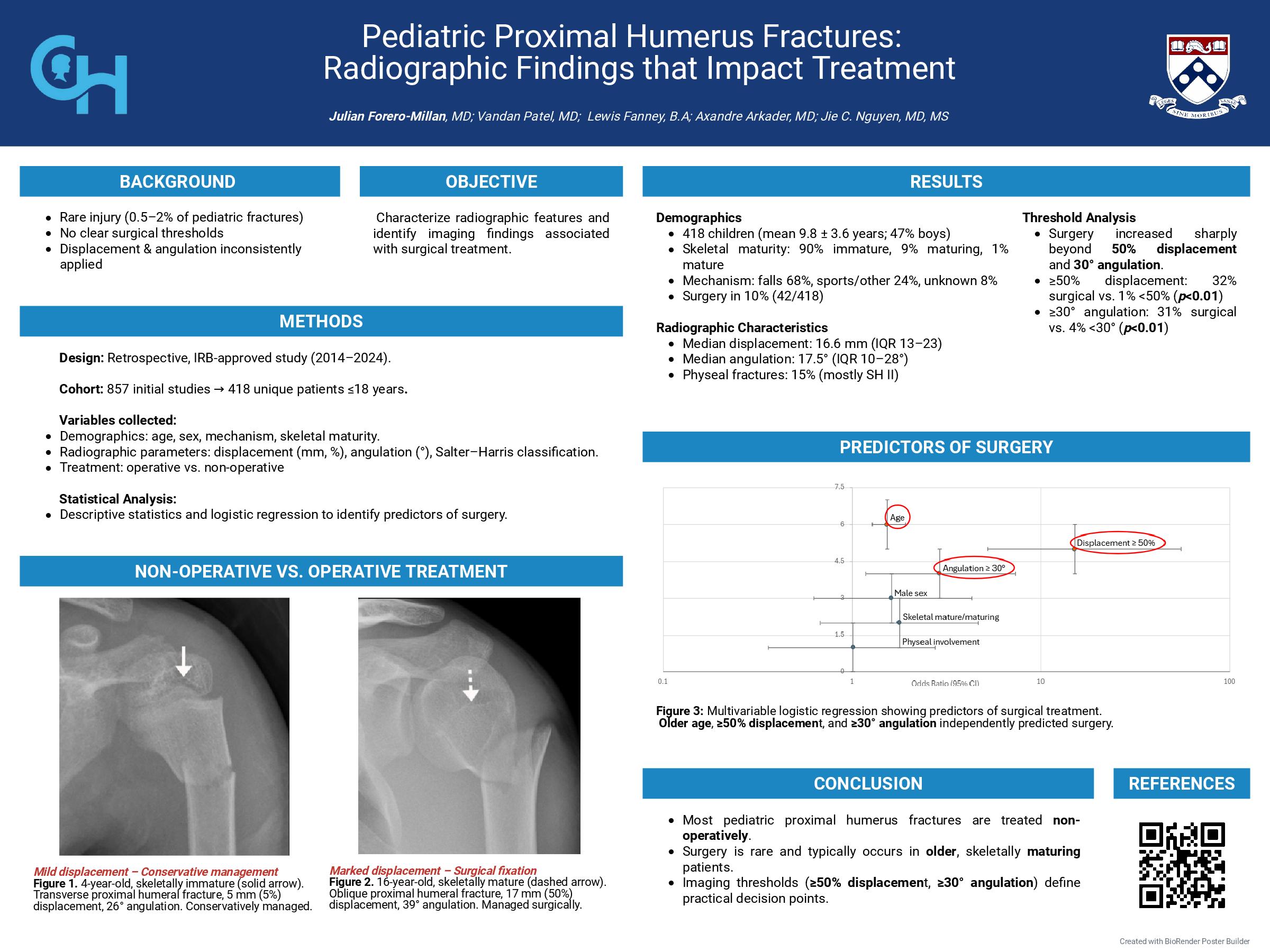
Methods & Materials: This IRB-approved retrospective case series included pediatric patients (≤18 years) with radiographically confirmed proximal humerus fractures over a 10-year period. Cases were identified by radiology report search using the terms “proximal humerus fracture,” “radiographs,” and “humerus.” Duplicates, patients >18 years, non-proximal fractures, and unconfirmed cases were excluded. Skeletal maturity, Salter-Harris pattern, maximum fracture displacement, angulation, and physeal involvement were collected along with demographics, injury mechanism, and treatment. Patients were categorized according to treatment as surgical or non-surgical (conservative management). Logistic regression was used to identify radiographic and clinical factors associated with surgical treatment; p<0.05 was considered statistically significant.
Results: In 418 included children (mean age 10.5±7.2 years, range, 1–17; 47% boys); 376 fractures occurred in skeletally immature, 37 in maturing, and 5 in mature shoulders. Physeal involvement occurred in 58 (15.4%) immature shoulders, predominantly Salter–Harris II (n=50, 86%). Median overall fracture displacement was 4.1mm (IQR, 2.0-11.2); relative displacement (percentage of shaft width) was 24% (IQR, 12-53%), and angulation was 17.5° (IQR, 10–28°). Among 380 patients with available follow-up radiographs, the median follow-up duration was 1.7 months (IQR, 1.0–2.5). Overall, 42 (10%) underwent surgery. Stepwise analysis found a significant association between surgery and ≥50 % displacement (33 % vs 1 %, p<0.01) and ≥30° angulation (33% vs 4%, p<0.01). On multivariable analysis, independent predictors of surgery included older age (OR, 1.53, 95% CI 1.28–1.92, p<0.01), ≥50% fracture displacement (OR 15.1, 95% CI 5.22–55.21, p<0.01), and angulation ≥30° (OR 2.91, 95% CI 1.18–7.36, p<0.02).
Conclusions: Fracture displacement ≥50% and angulation ≥30° were the strongest radiographic predictors of surgery in pediatric proximal humerus fractures, with older age also independently associated with operative management. Reporting these imaging findings can help guide clinical decision-making and surgical referral.
More abstracts on this topic:
Milks Kathryn, Whitaker Amanda, Mesi Erin, Ruess Lynne
Role of Pre-Hematopoietic Stem Cell Transplant Computed Tomography on Surveillance of Asymptomatic Infection and Air TrappingObermark Tyler, Debnath Pradipta, Trout Andrew, Ayyala Rama, Myers Kasiani, Tanimoto Aki, Danzinger-isakov Lara, Otto William, Morin Cara
Comments
We encourage you to join the discussion by posting your comments and questions below.
Presenters will be notified of your post so that they can respond as appropriate.
This discussion platform is provided to foster engagement, and stimulate conversation and knowledge sharing.
Please click here to review the full terms and conditions for engaging in the discussion, including refraining from product promotion and non-constructive feedback.
Please note that this is a separate login, not connected with your credentials used for the SPR main website.

Please note that this is a separate login, not connected with your credentials used for the SPR main website.